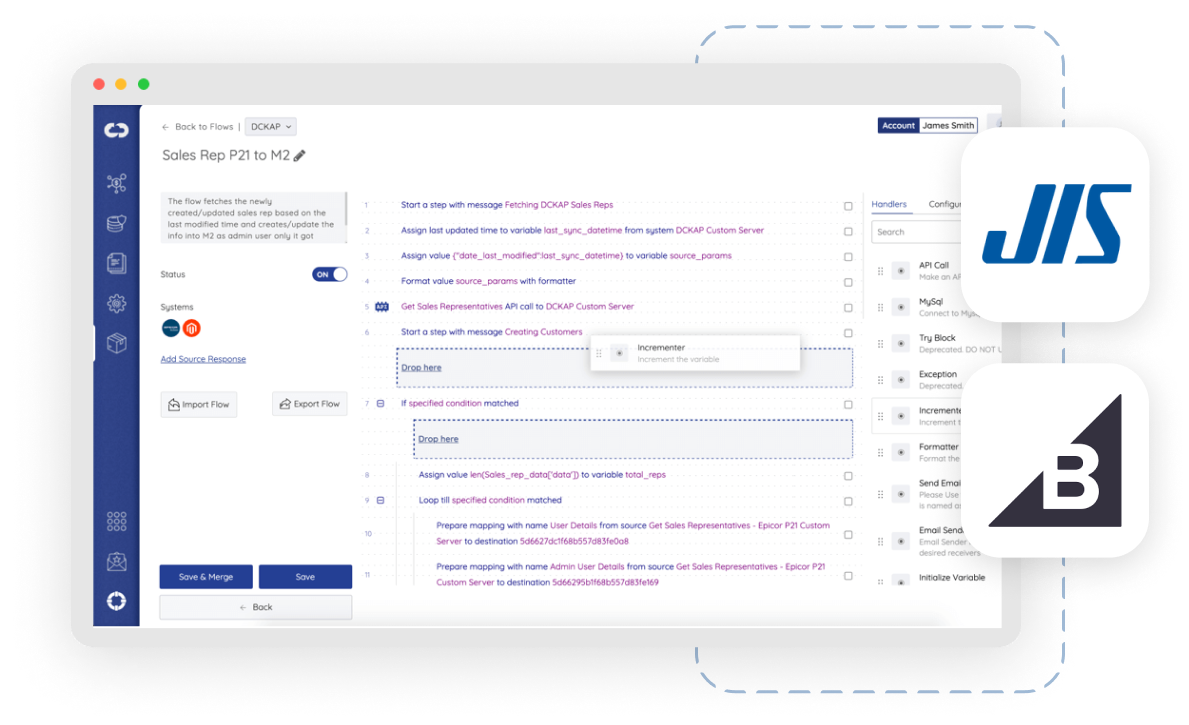
Stop jumping back and forth between systems. Connect, automate, and sync data between your CRM, ecommerce platforms, and popular ERPs such as Oracle Netsuite, Epicor Prophet 21, DDI Inform, Infor, Distribution One, Microsoft Dynamics 365, Sage & many more.